Healthcare is local. Providers understand the unique needs of their patients and the community. We offer these dedicated providers the benefits of a larger organization while enhancing independence.
Our Market Presence
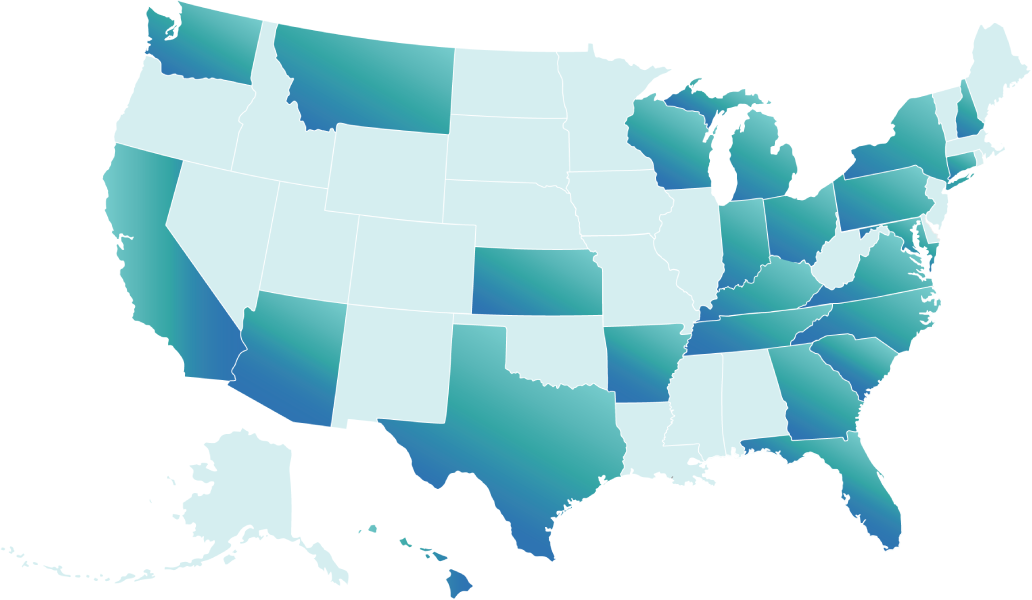
Click on your region to learn more.
Northeast
We unite, enable, and empower providers across Connecticut, Maryland, Virginia, Ohio and the District of Columbia. Our dedication to strengthening the patient-provider relationship and improving health and financial outcomes is unparalleled. Learn more to see if we are the right partner for you and your patients.
Mid-Atlantic Connecticut OhioCentral
United in providing lower-cost, higher-quality care to patients, our network is growing every day, and our physician groups excel with their extensive healthcare expertise. Explore our markets to learn how we’re transforming the healthcare delivery experience.
North Texas Gulf Coast Texas West Texas IndianaSoutheast
What began as a group of doctors joining forces to improve patient outcomes and advance value-based care has grown into one of the area’s most successful private practice physician organizations. Explore our Georgia, Florida, Tennessee, and North Carolina markets to see how we’re changing healthcare to help patients and providers.
Tennessee Georgia Florida North Carolina South CarolinaPacific
As we expand along the West Coast, we provide an alternative model for providers that is private practice from hospitals and health systems. Learn more about how we are using population health expertise, robust technology, and physician-led governance to improve patient care in communities across California and Washington.
California WASHINGTONDeveloping Markets
If you’re interested in our physician-led model, population health expertise, and innovative technology but don’t see your region on the map, please reach out to speak with one of our representatives.
Learn MoreInterested in putting your practice on the map in a new market?
Learn MoreFrequently Asked Questions
Privia partners with an anchor practice that has a strong reputation, physician leadership, and ability to embrace and amplify value-based care in their market. We then develop a network around leading primary care providers and specialists. Finally, we advance practice management, patient engagement, and value-based care initiatives. If you’re interested in becoming an anchor practice in a new market, please fill out this form to discuss a possible partnership.
Privia Women’s Health, our medical group custom-tailored to support OB-GYNs and their patients, spans across all markets. Privia Quality Network comprises our regional accountable care organizations (ACOs) in every market.
No. Privia partners with health systems to deliver a capital-efficient, forward-thinking, and diverse expansion strategy. We also partner with payers to reduce members’ utilization and costs while increasing engagement. Furthermore, we work with employers to develop employee benefits packages supported by our cost-efficient, high-quality provider network.