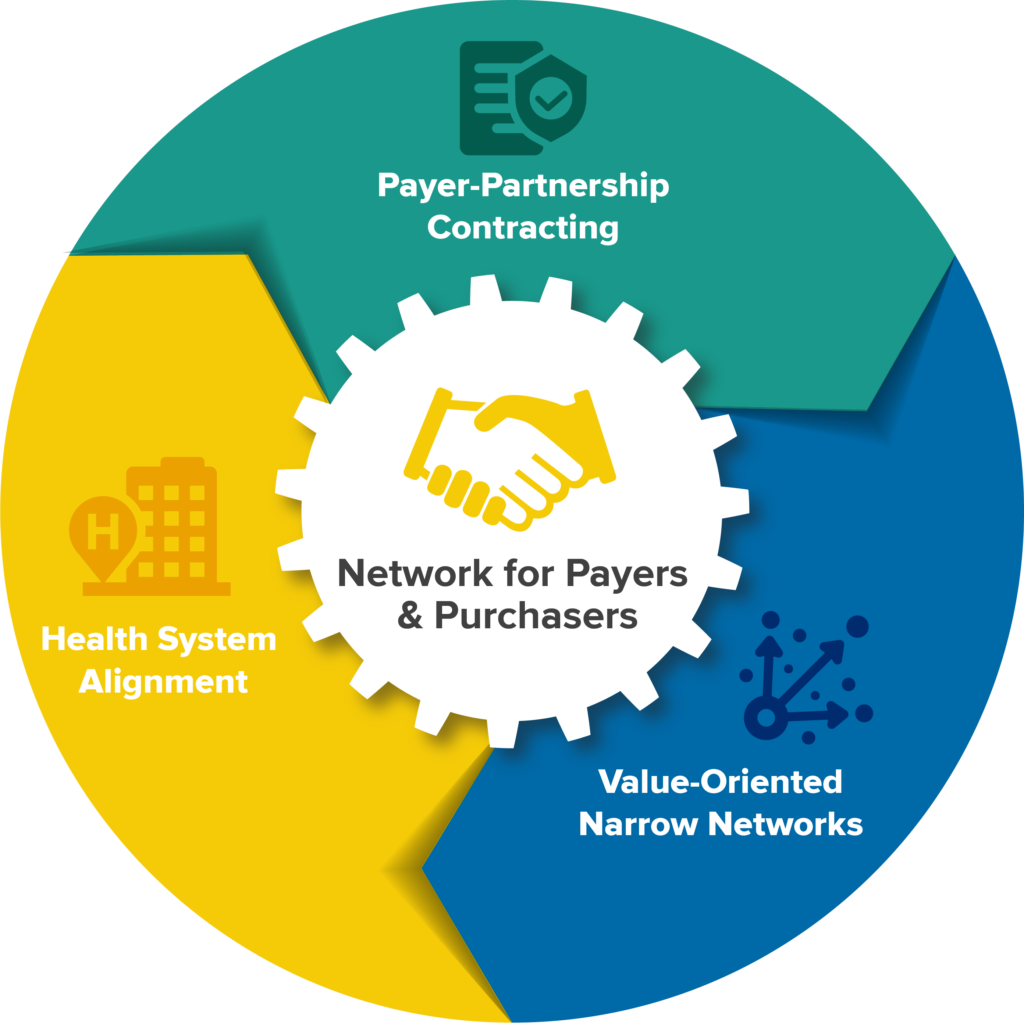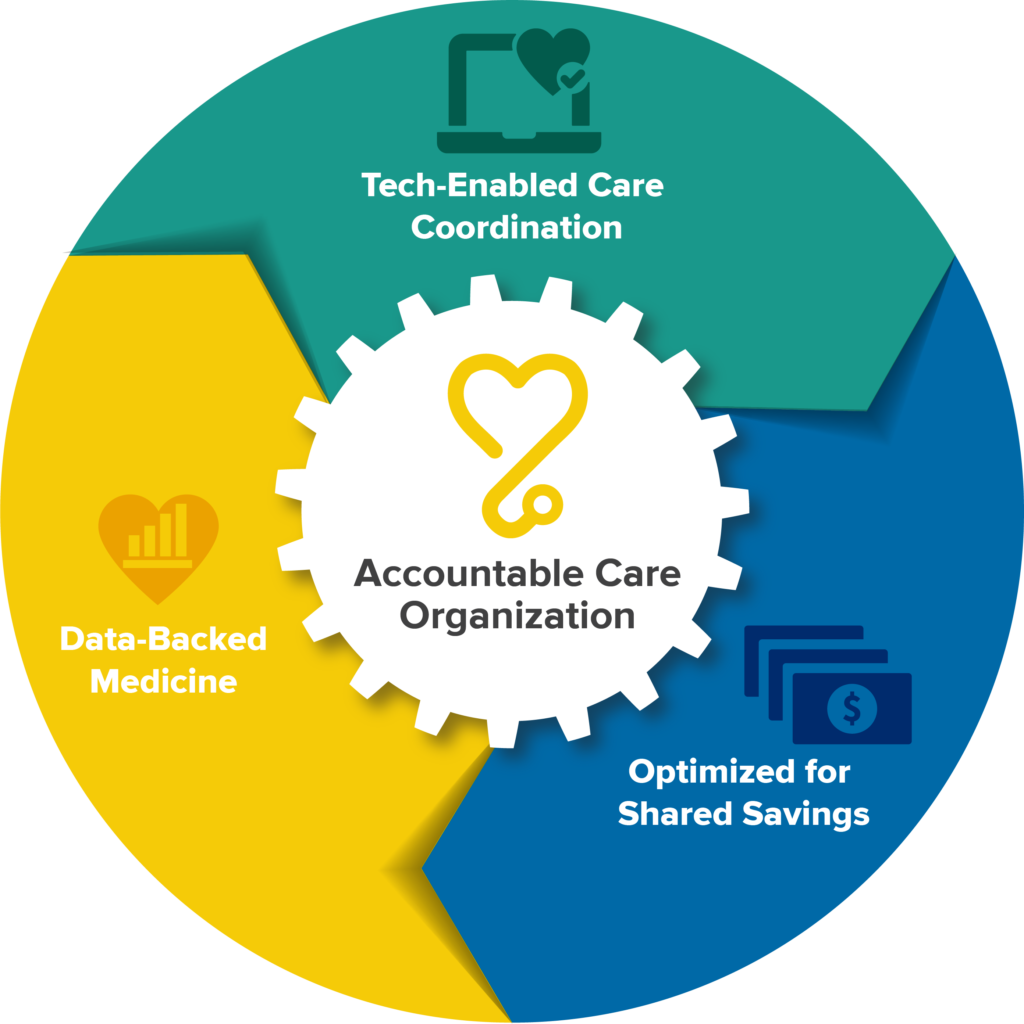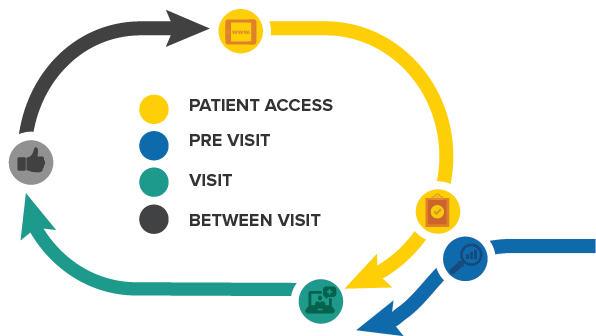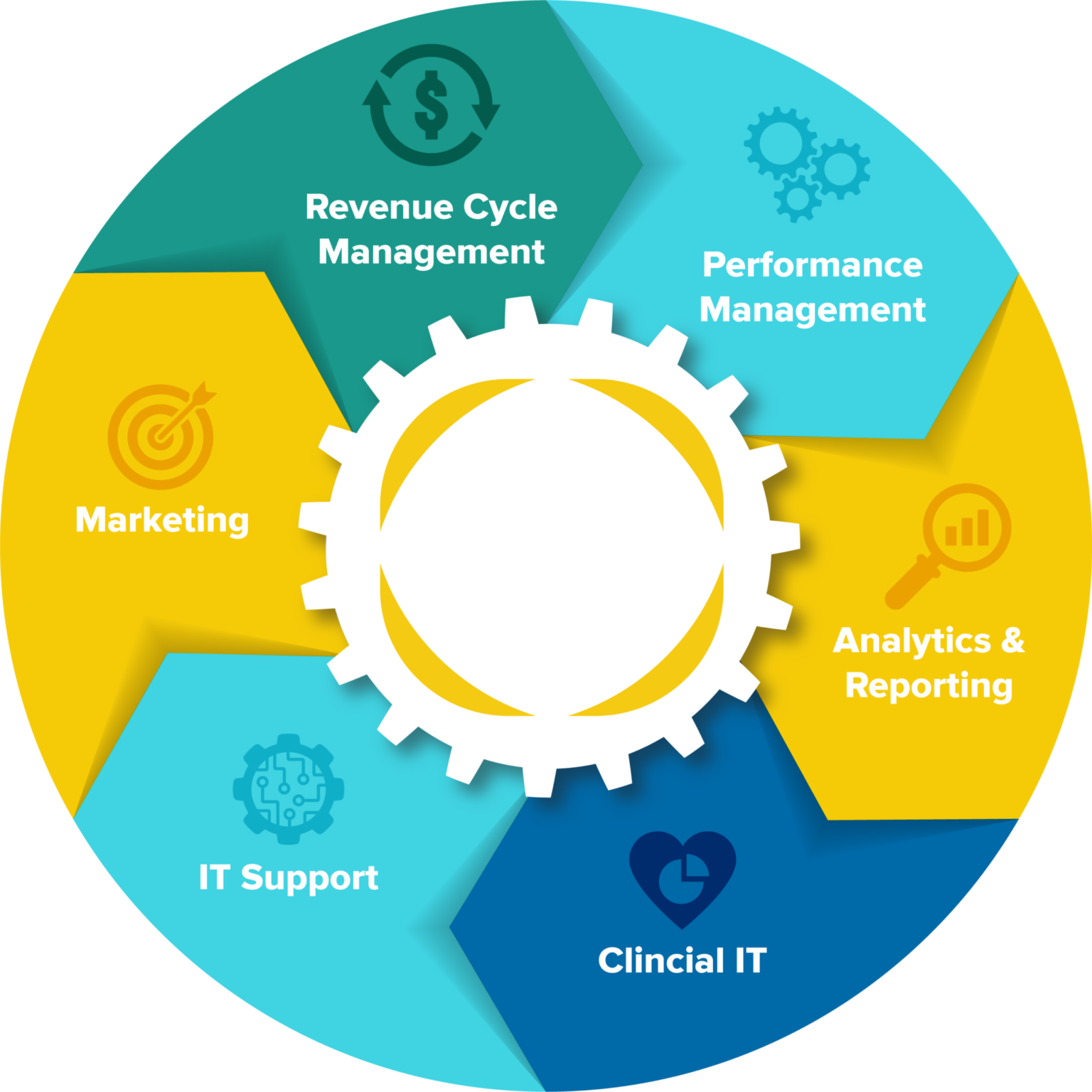
Management Services Organization (MSO)
Our MSO is designed to provide services that reduce administrative workloads, increase efficiency, and lower direct costs in practice operations. This framework can provide long-term revenue opportunities for our anchor partners.